 Showing patients their new Rx also removes “awkward conversation”
Showing patients their new Rx also removes “awkward conversation”
There’s a conversation that Keri Dennis, OD, no longer has with most patients. She isn’t put on the spot to make a judgment whether a patient “needs” new eyewear. Since she joined Ridgeview Eye Care in Olathe, Kansas, in August 2019, that’s one of the features that makes having Marco TRS automated refraction systems most enjoyable. It’s also why the practice added TRS systems to the new location in Lenexa, Kansas, that recently opened.
“Being able to show patients the difference between their habitual prescription and the one from that day’s exam is one of the most valuable aspects. Being able to toggle back and forth between the two helps patients see for themselves if it’s valuable to purchase new eyewear,” she says.
It removes an “awkward conversation” from the patient encounter, but it also adds efficiency to the process. In the original Olathe office, two of the three exam lanes have the TRS system. The third is dedicated primarily to pediatric patients. “When I’m working, I want one of the rooms with a TRS,” she says, laughing.
The technicians who conduct the pretesting insert a card into the TRS system that provides the data. There are no transcription errors or time spent dialing in refractions. “It saves our technicians time and reduces errors, and all of those factors add up to speed and efficiency. Patients love that,” she says.
It’s not that they’re necessarily in a rush to get through their exam, but most patients found the old refractions – which is better? – frustrating.
“Patients want a modern practice to have modern technology. If they come here from an office that did not have it, they say, ‘Wow. I’ve never seen this before.’ We get that all the time.”
A little social distance
An unexpected benefit of having the TRS systems in place during and right after COVID-19 was the fact that she could complete her refractions with some social distancing. “The timing of having these systems in place then was have to lean right in and spin dials,” she says.
There are also ergonomic and efficiency advantages to this system. Because she can control the automated refraction system from a tabletop device, she can go home with no shoulder or neck pain at the end of the day. “It’s also a faster process because I don’t have to turn around from the phoropter and write down notes. In fact, I can do quite a bit of multitasking because I can pull up optical coherence tomography scans and images. While I’m doing the refraction, I can look at data that can help me determine if there’s something else affecting their vision. It’s a more streamlined process because I’m not sitting in front of the patient spinning dials,” she says.
With three doctors working at the same time, each moment that the patient is in an exam lane is valuable. So being able to use the time that might otherwise be spent in the manual refraction process to gather data that supports her clinical decisions is important.
Patients also appreciate being able to get through the process without the stress or extra time involved. With the added benefit of being able to show them their previous and new prescriptions, the practice
is capturing more eyewear sales. “It absolutely makes a difference because it’s difficult for patients to assess whether an updated prescription would be better if we need to dial the comparison in. We find that if patients detect an improvement of any sort in these TRS comparisons, it improves the capture rate tremendously.”
Growing practices
The practice opened its Lenexa location in an area of rapid commercial and residential growth. Having advanced technology that wows patients is an important part of the attraction, she says. Patients want a whole experience at their eye care provider’s office-from a beautiful location, friendly staff and the expectation that they are getting a thorough and efficient eye exam.
Being able to provide that from the start in both offices contributes to the culture of excellence and efficiency, evidenced through the practice’s nearly 5-star Google reviews.
Article originally published in Vision Source OD magazine. Learn more about Vision Source here.




 Of her three exam lanes at
Of her three exam lanes at 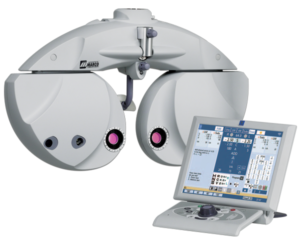
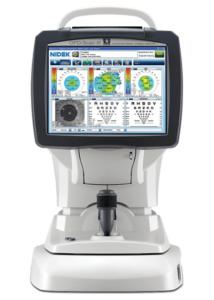
 One of the first investments that Michelle McReynolds, OD, made when she opened cold was with the Marco OPD Scan III Wavefront Aberrometer and TRS automated refraction system. “I was looking for anything that would make my work faster because I didn’t have a technician when I first opened. It was just me doing everything,” she recalls. She opened West County Vision Center in St. Louis, Missouri, in 2011.
One of the first investments that Michelle McReynolds, OD, made when she opened cold was with the Marco OPD Scan III Wavefront Aberrometer and TRS automated refraction system. “I was looking for anything that would make my work faster because I didn’t have a technician when I first opened. It was just me doing everything,” she recalls. She opened West County Vision Center in St. Louis, Missouri, in 2011.


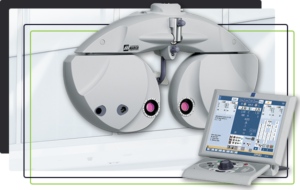

 Kathleen Joyce, OD, of EYECARE for You, makes a firm distinction between the different automated refraction systems out there. “My refractions are doctor-driven, but I love having the technology that helps me get to an accurate subjective refraction more quickly,” she says. That is important to her in her two practice locations where she focuses on medical services and custom fit contact lenses. “The refraction is a pivotal part of the exam, and my
Kathleen Joyce, OD, of EYECARE for You, makes a firm distinction between the different automated refraction systems out there. “My refractions are doctor-driven, but I love having the technology that helps me get to an accurate subjective refraction more quickly,” she says. That is important to her in her two practice locations where she focuses on medical services and custom fit contact lenses. “The refraction is a pivotal part of the exam, and my 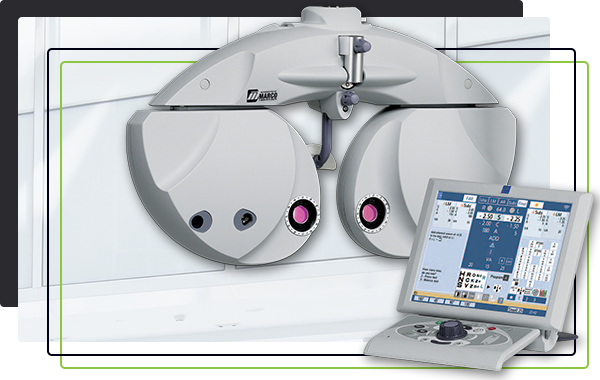

 After about nine years of having an automated refraction system in the practice, Heavin Maier, OD, of Eyes for Life in Spokane, Washington, couldn’t imagine practicing without it. When she added another lane of equipment, the Marco
After about nine years of having an automated refraction system in the practice, Heavin Maier, OD, of Eyes for Life in Spokane, Washington, couldn’t imagine practicing without it. When she added another lane of equipment, the Marco 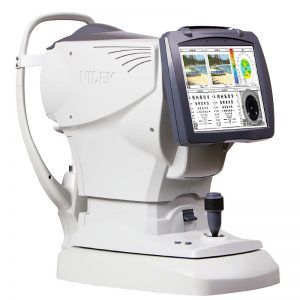 The patient experience
The patient experience
 One of my favorite exercises for doctors to learn how their office operates is to first have each staff member take a guess (doctors too!) at how long the patient spends at each part of their patient journey. This includes check-in, waiting room, pre-testing, waiting in the exam room for the doctor, the eye exam, optical time, and checkout. I call this the “Post-It Note” exercise, as we would write the time that the patient started and completed each step on a post-it note.
One of my favorite exercises for doctors to learn how their office operates is to first have each staff member take a guess (doctors too!) at how long the patient spends at each part of their patient journey. This includes check-in, waiting room, pre-testing, waiting in the exam room for the doctor, the eye exam, optical time, and checkout. I call this the “Post-It Note” exercise, as we would write the time that the patient started and completed each step on a post-it note. Once the patient is done in the exam room, streamlining the handoff to optical can expedite the process. Can you directly send all relevant information to your opticians, including prescription(s), lens recommendations, and treatments so they automatically have that information when the patient arrives?
Once the patient is done in the exam room, streamlining the handoff to optical can expedite the process. Can you directly send all relevant information to your opticians, including prescription(s), lens recommendations, and treatments so they automatically have that information when the patient arrives?
 Claudio Lagunas, OD, is a builder of practices. He has owned nine—with four at one time—but now has just two. One is his established practice in Woodlands, Texas. He and his wife Grisel Lagunas, OD, recently acquired an existing practice in Spring, Texas, when the opportunity was too good not to jump at it.
Claudio Lagunas, OD, is a builder of practices. He has owned nine—with four at one time—but now has just two. One is his established practice in Woodlands, Texas. He and his wife Grisel Lagunas, OD, recently acquired an existing practice in Spring, Texas, when the opportunity was too good not to jump at it.
 Automated system for refractions brings physical relief, too.
Automated system for refractions brings physical relief, too.

